If you’re considering Wegovy as part of your weight management journey, you might be wondering: Does Priority Health cover Wegovy? The answer depends on several factors, including your specific plan, medical necessity, and prior authorization requirements. In this article, we’ll explore what Wegovy is, how Priority Health handles coverage, and what steps you can take to increase your chances of approval.
What is Wegovy?
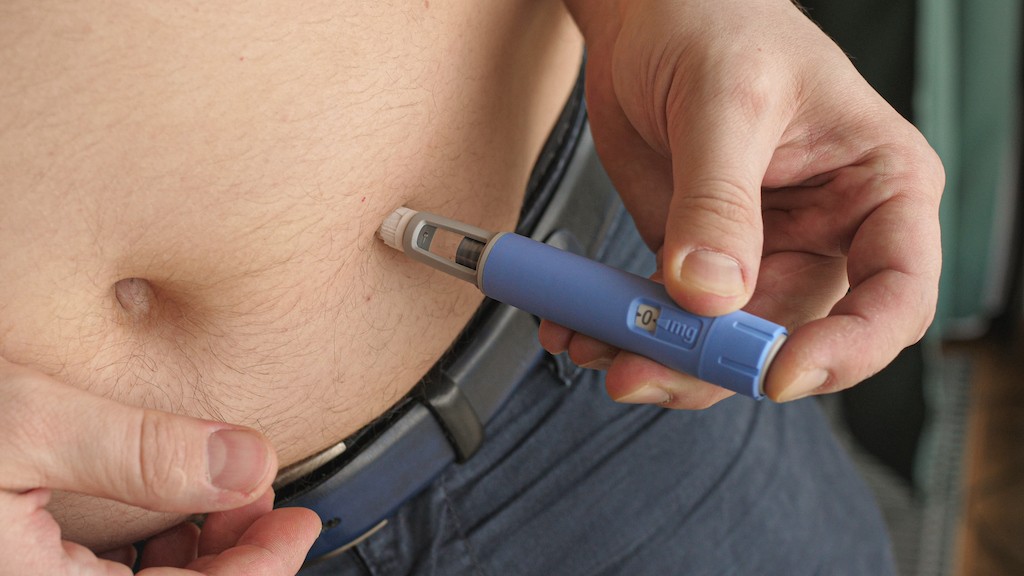
Wegovy (semaglutide) is an FDA-approved prescription medication designed to help adults with obesity or those overweight with weight-related health conditions lose weight and maintain weight loss. It works by mimicking a hormone called GLP-1 (glucagon-like peptide-1) that regulates appetite and food intake.
Does Priority Health Cover Wegovy?
Priority Health may cover Wegovy under certain plans, but coverage is not guaranteed. Like many insurers, Priority Health typically considers weight-loss medications to be optional, and coverage often depends on:
- Type of Plan: Employer-sponsored, individual, or Medicaid/Medicare plans may have different rules.
- Medical Necessity: You may need to meet BMI criteria (usually BMI ≥30 or BMI ≥27 with related conditions like type 2 diabetes, hypertension, or sleep apnea).
- Prior Authorization: Your doctor may need to submit documentation proving that Wegovy is medically necessary and that other weight-loss methods have been tried without success.
Steps to Determine If Your Plan Covers Wegovy
- Check Your Plan Documents: Review your Priority Health formulary (drug list) to see if Wegovy is listed.
- Contact Customer Service: Call the number on your Priority Health ID card and ask about coverage for Wegovy (semaglutide).
- Ask About Requirements: Inquire about prior authorization, step therapy, and coverage limitations.
- Work with Your Doctor: If prior authorization is needed, your healthcare provider can submit the necessary forms and supporting medical records.
Why Might Priority Health Deny Wegovy Coverage?
Common reasons for denial include:
- The medication is not on your plan’s formulary.
- Lack of documented medical necessity.
- Failure to meet BMI or health condition requirements.
- Not completing prior authorization or step therapy processes.
What Are Your Options If Coverage Is Denied?
- Appeal the Decision: You can request a formal review of the denial with additional medical documentation.
- Patient Assistance Programs: Novo Nordisk, the manufacturer of Wegovy, offers financial assistance programs for eligible patients.
- Alternative Medications: Ask your doctor about other GLP-1 medications or weight management options that might be covered.
Conclusion
So, does Priority Health cover Wegovy? The short answer is: possibly, depending on your plan and medical needs. Always review your policy, consult your doctor, and contact Priority Health directly to confirm coverage details. With the right preparation, you can improve your chances of accessing this effective weight-loss treatment.